Moving SBRT From Selected Cases to Standard Practice.
SBRT delivers treatment in fewer, higher-dose fractions. But higher dose per fraction demands higher geometric certainty during delivery. Without it, margins stay wide and the advantage of fewer fractions is lost to higher risk for side effects. The Raypilot® System provides the geometric certainty needed for hypofractionated SBRT. The evidence below shows the results.
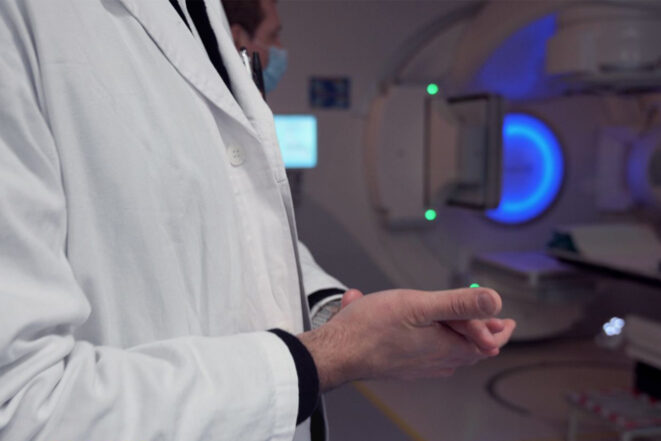
Why SBRT, and Why Now?
Prostate radiotherapy has traditionally required 20 to 39 sessions over up to two months. SBRT compresses that into 3–5 fractions. But concentrating the dose demands proportionally greater control over where that dose lands. Reducing fractions without improving geometric precision during delivery is a compromise, not an advance. That geometric control is now available. The studies below represent the clinical evidence base for prostate SBRT, including the largest randomised trials to date and real-world outcomes from clinics treating with the Raypilot® System.
Outlining of urethra
Reproducibility of bladder filling
Right dose delivered to right target
Evidence and Key Clinical Studies
View all publicationsPACE-B: Phase 3 trial of SBRT in localised prostate cancer
874 patients randomised to SBRT (5 fractions) or moderate hypofactionation or conventional fractionation (20 or 39 fractions). SBRT demonstrated non-inferiority for biochemical or clinical failure, reducing treatment from 4 weeks to 1–2 weeks with no increase in late toxicity.
Why it matters: This is the largest randomised trial confirming SBRT as a standard of care. With The Raypilot System's continuous motion tracking, margins can be tightened further, supporting the move from selected cases to routine practice.
Read our summaryPACE-C: Moderate hypofractionation vs. SBRT, early toxicity
Head-to-head comparison of moderate hypofractionation and SBRT. Early toxicity results confirm that the increased toxicity seen with SBRT is predominantly urethra-related; the exact issue that The Raypilot System's urethra visualisation addresses. moderate hypofractionation and SBRT
Why it matters: The residual toxicity risk in SBRT is manageable with the right tools. Urethra-sparing technique is the key, and that requires knowing where the urethra is during delivery
Read our summaryABRUPT: Toxicity and quality of life with dose-escalated SBRT using The Raypilot System
Prospective study of ablative radiotherapy for unfavourable prostate tumours with The Raypilot System, using one single fraction. Reports toxicity rates and quality-of-life outcomes at dose escalation.
Why it matters: Raypilot System-specific clinical data. Measured outcomes from patients treated with this system in routine clinical practice.
Read our summaryIntrafraction Motion Management: Different Approaches
Several technologies address intrafraction prostate motion. The Raypilot® System and MR-guided radiotherapy take fundamentally different approaches, each with distinct characteristics in terms of workflow, infrastructure, and clinical integration. Both approaches address a real clinical need. The choice depends on clinical priorities, patient volume, and existing infrastructure.
| Raypilot® System | MR-guided RT | |
|---|---|---|
| Tracking method | Electromagnetic, 30 Hz, continuous | MR imaging, cine acquisition |
| Treatment time / fraction | 15 min | 40–60 min |
| Infrastructure | Installs on existing linac | Dedicated suite with RF shielding |
| Soft tissue visualisation | Urethra (via Raypilot Hypocath) | Full soft-tissue contrast |
| Capital investment | Add-on system | Standalone system |
Treatment Workflow using the Raypilot® System
The Raypilot® System fits into a standard SBRT workflow without requiring a new equipment room or scheduling infrastructure. Below is what changes, and what stays the same.
CT with Raypilot Viewcath
Raypilot Viewcath inserted, CT acquired, urethra outlined. Removed same session.
Schedule
Patient scheduled for treatment.
Raypilot Hypocath insertion
Standard catheterisation. Bladder filled to planned volume.
~15 min / fraction
Real-time 3D tracking. Beam gated to tolerance. 1–5 fractions.
Raypilot Hypocath removed
Patient goes home. Routine follow-up.
Interested in Bringing SBRT to Your Clinic?
The Raypilot® System is in clinical use at centres across Europe. Get in touch to discuss implementation, visit a reference clinic, or learn more about integrating SBRT into your treatment offering.
Downloads
View all downloadsThe Raypilot® System Flyer
An overview of The Raypilot® System for intrafraction motion management, featuring system components, key clinical benefits, and references from treating clinicians.
Download Raypilot System FlyerThe Raypilot® System Technical Flyer
Technical specifications for The Raypilot® System, including receiver dimensions, catheter specifications, position update performance, and measurement precision data.
Download Raypilot System Technical FlyerFrequently Asked Questions
View all FAQs-
How does urethra visualization reduce side effect?
The urethra is considered an organ at risk and should be spared from unnecessary radiation exposure. As the urethra passes through the prostate and is not itself diseased, minimizing the radiation dose to the urethra is important to reduce the risk of treatment-related side effects. Lower dose exposure to organs at risk, such as the urethra, is associated with improved safety and reduced toxicity.
-
Is SBRT with the Raypilot System suitable for all risk groups?
For organ defined prostate cancer yes.
-
What does a typical SBRT workflow with the Raypilot System look like?
It starts with a CT or MRI simulation with the simulation catheter Raypilot Viewcath. On the first treatment day the Raypilot Hypocath is inserted followed by concequtive 1-5 days treatment. Raypilot Hypocath ensure motion tracking for the user to stop the beam if necessary.
-
What level of evidence supports SBRT for prostate cancer Treatment?
Following an intermediate cancer there are several studies and experience using SBRT for Prostate Cancer treatment, for example HYPO-RT, PACE-B, FLAME and ongoing PACE-C study. SBRT has been used for 10 years.
Ready to See How It Works in Practice?
Talk to our team about clinical workflows, the implementation process, or visit one of the clinics already treating with The Raypilot® System. Reach out to us to learn more.